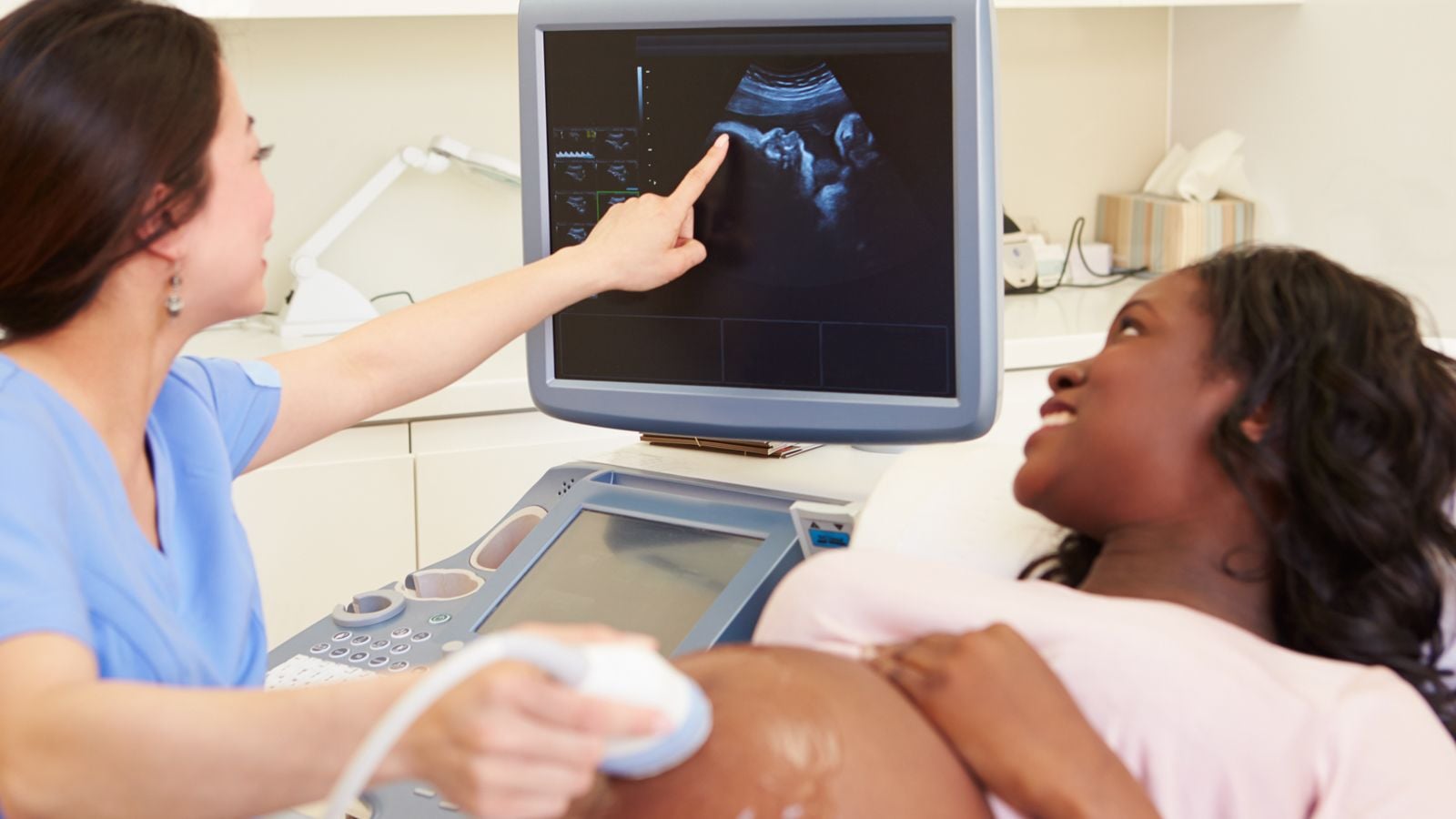
A baby growing in its mother’s uterus is surrounded by a sac containing amniotic fluid, which serves several vital functions. The fluid protectively cushions the developing fetus, helps to prevent infection, maintains a constant temperature inside the womb, gives the baby room to move around, which is needed to enable proper muscle and bone growth, and provides fluids necessary for the baby’s digestive and respiratory systems to develop. As the baby grows, it breathes the amniotic fluid into its lungs, swallows some, and then excretes it as urine to keep the volume of amniotic fluid steady. Initially, amniotic fluid is made up largely of water and other fluids provided by the mother; later in the pregnancy, most of the fluid is actually comprised of fetal urine. Sometimes, too much amniotic fluid builds up in the womb – this condition is called polyhydramnios and usually happens during the second half of pregnancy. Polyhydramnios (sometimes called just hydramnios) occurs in only about 2% of pregnancies.
Why Do Some Women Get Polyhydramnios?
Specific causes of polyhydramnios generally cannot be determined in about 2/3s of cases. When a cause can be traced, among the common reasons are poorly-controlled maternal diabetes, twin or multiple gestations (especially when one twin has too little amniotic fluid and the other produces too much, referred to as twin-to-twin transfusion syndrome), fetal abnormalities which make it difficult for the baby to swallow and process the fluid normally (e.g., a cleft lip or palate, gastrointestinal blockage, hydrocephaly, or other neurological problems or heart defects), Rh blood incompatibility, which can bring on fetal anemia and other factors.
Many occurrences of polyhydramnios resolve on their own without causing any pregnancy complications. Other women, however, may experience abdominal discomfort and breathing problems from fluid buildup that exerts pressure on the lungs and other internal organs. The most serious potential risks produced by polyhydramnios are the possibility of premature rupturing of the amniotic sac, early labor, and delivery and/or placental abruption (placenta separating from the uterine wall before delivery) or umbilical cord accidents. The presence of extra amniotic fluid also increases the possibility of postpartum bleeding, if the mother’s uterus is too stretched out to properly contract after delivery.
Treatment Options for Polyhydramnios:
With careful monitoring, many cases of polyhydramnios are easily treated and present no serious threat to either the baby or the mother.
Ultrasound
If a woman is diagnosed with polyhydramnios, she is checked with a high-resolution ultrasound, to make sure the baby is growing at a normal rate. Further ultrasounds are performed regularly during the pregnancy to ensure that the excess amniotic fluid is not having a detrimental effect on the baby’s development.
Amniocentesis
An expectant mother with polyhydramnios will also be watched closely for signs of preterm labor. If her doctor feels that the presence of too much fluid might be problematic, some can be safely removed through a process called amnioreduction, which is done through amniocentesis. However, amniocentesis itself can sometimes cause problems, and it’s possible for polyhydramnios to recur even after some fluid has been drained out.
Medication
Medication can also be administered to reduce the amount of amniotic fluid, but this treatment approach is used only until the 32nd week of pregnancy to avoid further complications. If a pregnant woman has diabetes, this increases the risk that she’ll develop polyhydramnios, so careful attention must be paid to her sugar levels; treating high blood sugar levels often reduces the volume of amniotic fluid and can help resolve the situation. In rare, extreme cases of polyhydramnios, a baby might be delivered in advance of its due date if the doctor is concerned that the excess amniotic fluid poses a developmental threat.